Caption
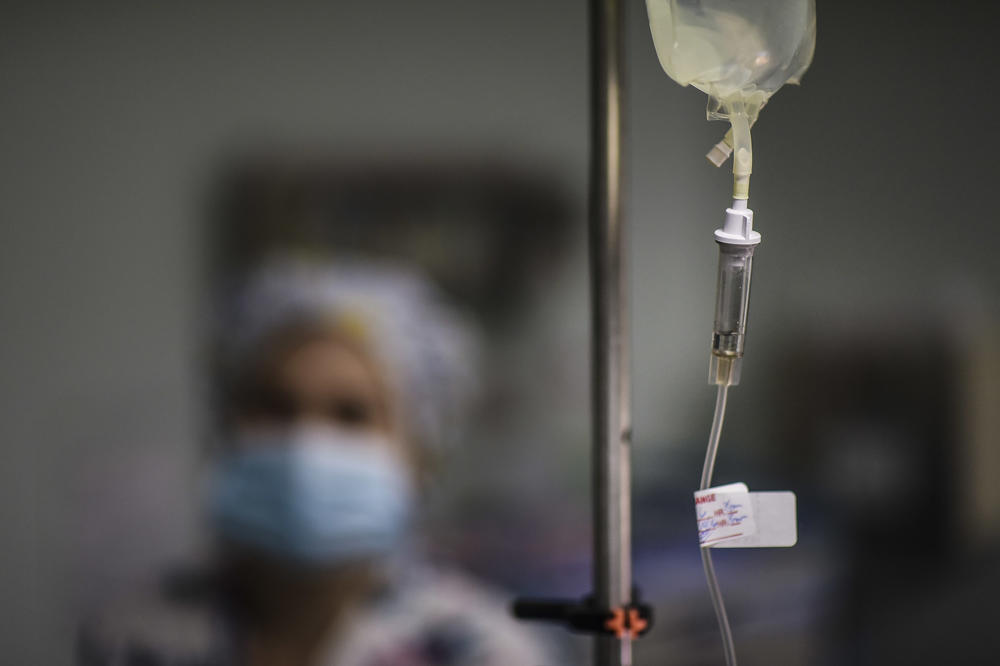
Emory Healthcare, like nearly every health care organization in the area and across the country, is facing staffing challenges for nursing and other clinical positions, says Emory CEO Jonathan Lewin.
Credit: Tristan Smith/GPB News