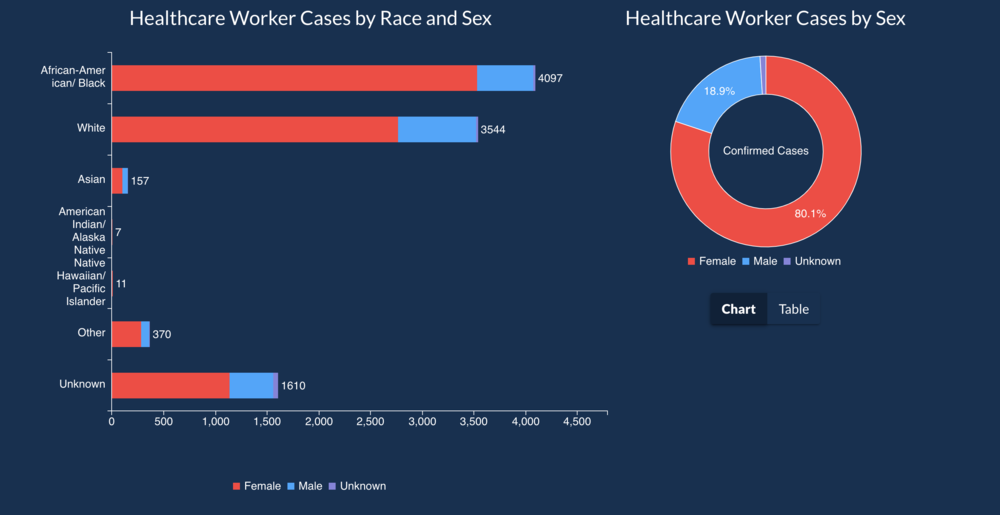
Caption
Emory Healthcare CEO Jonathan Lewin earlier this month said he was concerned for his employees' mental health. "It is tough to keep morale up when we see people, our fellow citizens, could be preventing this, but aren’t," he said.
Credit: Tristan Smith/GPB News